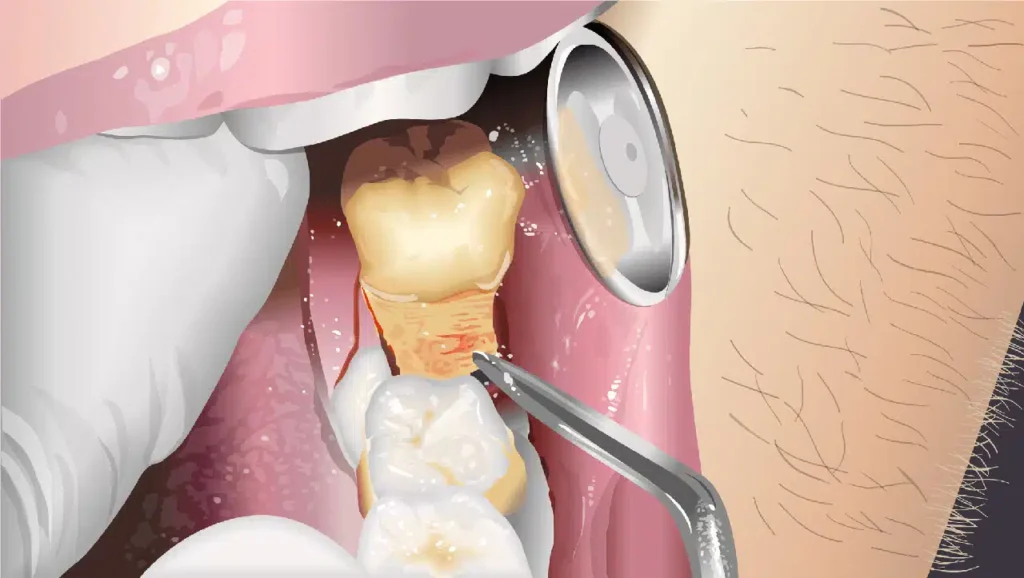
What is a wisdom tooth extraction?
Wisdom tooth extraction is a common procedure in oral surgery. The third molar, which erupts later in life, often fails to erupt properly due to a lack of space. In many cases, a lower or upper wisdom tooth is removed for preventive purposes.
Thanks to advances in techniques and technology, it is now possible to carry out this procedure in an atraumatic way, minimizing post-operative pain and speeding up recovery times. The extraction of a wisdom tooth (lower or upper) is usually performed using forceps and controlled force to loosen the tooth from the surrounding tissues, allowing its removal. The issue with this technique is the duration of the procedure and the potential fracture of the tooth roots, which may require a more complex and invasive surgical session.
No more anxiety or fear about wisdom tooth extraction.
When should wisdom teeth be removed?
Not all wisdom teeth need to be extracted. They are often removed preventively to avoid infections, decay that may also affect the second molar, pericoronitis, or cysts. Since wisdom teeth do not play a significant role in chewing, it is generally appropriate to remove them at the first sign of problems.
If a wisdom tooth erupts in a misaligned position, and considering how difficult it is to reach with a toothbrush, it can easily develop decay and lead to infections. Extraction of an upper or lower wisdom tooth is necessary in the presence of:
Decayed wisdom teeth
The extraction of a decayed wisdom tooth is often necessary due to its posterior position, which makes proper oral hygiene difficult. Food debris is frequently not effectively removed by brushing and flossing.
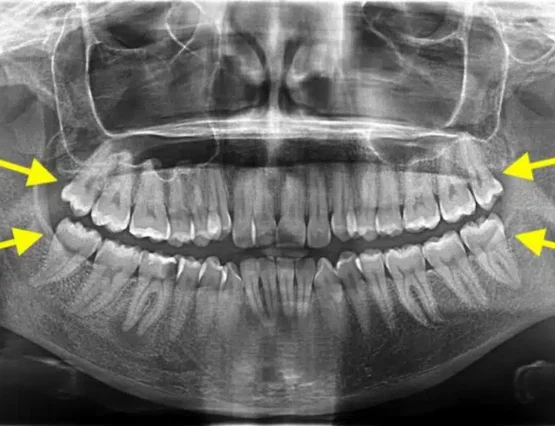
The extraction of a decayed upper wisdom tooth often requires the removal of the corresponding lower one as well. Otherwise, over time, the lower tooth may over-erupt due to the lack of an opposing tooth, leading to food accumulation from loss of contact point and potential decay of the second molar.
Impacted tooth
The tooth may remain partially or completely trapped in the gum or bone. Should an impacted wisdom tooth be removed? Not necessarily. If the follicular sac surrounding the crown is intact, the tooth is not tilted toward the second molar (thus not risking damage), and there are no symptoms, extraction may not be required.
Early extraction
Early removal of wisdom teeth is often recommended to prevent more complex extractions in the future. The current approach tends to favor removing potentially problematic wisdom teeth before complications arise.
Infections and decay
Difficulty in cleaning these areas can lead to severe decay or pericoronitis (gum infections). Bacterial buildup in such hard-to-reach zones can make these conditions chronic if not treated promptly.
Abnormal orientation
Wisdom teeth often erupt horizontally due to lack of space, exerting pressure on adjacent teeth. This can cause pain and lead to decay on the distal surface of the second molars.
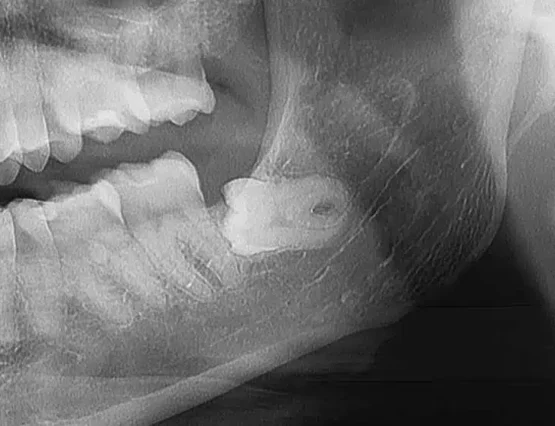
These, moreover, are very difficult teeth to treat. In such cases, preventive extraction of the wisdom tooth is recommended.

Dr. Fabio Cozzolino is the author of this guide. He specializes in periodontitis, dental implants, and atraumatic tooth extractions. He has published numerous studies and has perfected the extraction technique without forceps, relying solely on elevators.
Classification of dental extractions
Wisdom tooth extractions are not all the same, and there are significant challenges to address, such as in the case of impacted, partially impacted teeth, or teeth close to the inferior alveolar nerve. Extractions are divided into two categories:
Simple extraction (erupted teeth)
The tooth, or its remaining portion, is still present in the dental arch and/or easily accessible to the surgeon, and its removal is not complicated by particular anatomical conditions (such as curved roots or proximity to nerves).
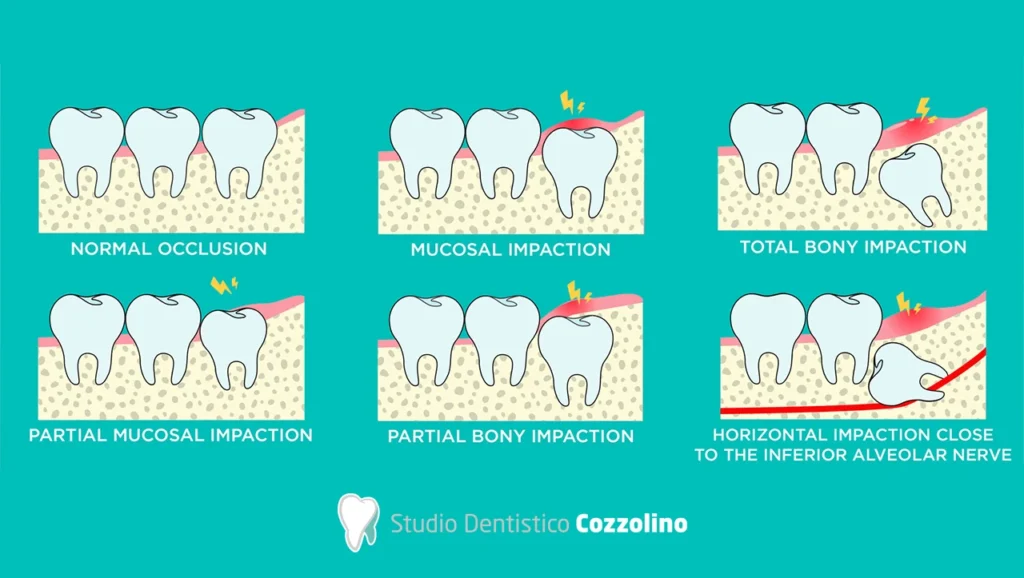
Complex extraction (impacted and partially impacted teeth)
Surgical extraction of wisdom teeth is performed when the tooth is partially or completely covered by bone and gum tissue. This includes cases of partial impaction and soft tissue impaction, as well as partial or complete bony impaction.
Wisdom tooth extraction is often further complicated by curved roots and proximity to the inferior alveolar nerve. In these cases, a more advanced and complex surgical approach is required.
Diagnosis and preliminary assessment
Third molars should be evaluated between the ages of 14 and 16 to assess available space and ensure proper eruption. Pre-extraction evaluation includes radiographic examination, panoramic X-rays, and computed tomography (CT scan). This allows for a three-dimensional view, making it possible to identify the nerve and accurately plan the procedure.
This is essential to minimize surgical risks. Extraction of lower wisdom teeth requires a high level of clinical expertise due to their proximity to the inferior alveolar nerve and the lingual artery. The inferior alveolar nerve (IAN) provides sensation to the lower jaw and lip. Sonic instruments help reduce the risk of paresthesia and accidental injury to the inferior alveolar nerve, lingual nerve, or surrounding arteries.
3D diagnostics (CBCT) and digital planning
Before surgery, Cone Beam Computed Tomography (CBCT) is used to map the position of the inferior alveolar nerve (IAN). This pre-operative assessment allows for precise surgical planning, helping to avoid neurological risks such as paresthesia.
Today, these data can be integrated into computer-guided surgical templates, enabling the surgeon to operate with pre-planned, millimeter-level precision while minimizing the extent of surgical incisions.
Advanced technologies for faster extraction
Local anesthesia is administered to prevent pain. For lower molars, three injections are typically required: one inferior alveolar nerve block and two infiltrations for the buccal and lingual nerves. The extraction of a wisdom tooth (upper or lower) is usually performed like that of any other permanent tooth: using forceps to apply controlled force, loosening the tooth from the surrounding tissues to allow removal.
The main issue with this technique is the potential fracture of the tooth, which may lead to a longer surgical procedure. Pain-free wisdom tooth extraction can also be performed using an elevator instead of forceps. How long does it take? Unless there are abnormal positions, the procedure takes only a few seconds: it is atraumatic, with a lower risk of root fracture and no significant complications. Here is the procedure we follow for pain-free wisdom tooth extraction using the elevator technique:
EWF Technique (Extraction Without Forceps)
Instead of using traditional dental forceps to pull the wisdom tooth, elevators are used. These are inserted between the tooth and the alveolar bone. This allows the use of leverage to multiply the applied force, making the extraction more efficient and less traumatic. In addition to loosening the tooth from the socket, with this technique the elevators can complete the entire extraction. Elevators reduce the risk of root fracture. By applying force at a single point, they guide the tooth in the direction of least resistance. Forceps, on the other hand, force the tooth in a predetermined direction, increasing the risk of root fracture. With elevators, even when roots are significantly curved, it is often possible to avoid breaking the tooth—preventing the need for a more invasive procedure involving bone removal to extract the root apex.
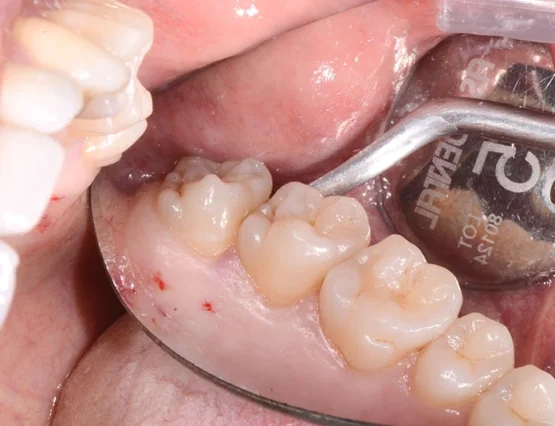
The extraction is often completed in just a few seconds, reducing pain, healing time, and significantly lowering the amount of force perceived by the patient compared to the use of forceps. The atraumatic extraction technique using elevators instead of forceps has been thoroughly described and expanded upon in the medical journal Zerodonto, specifically in the article “Extraction Without Forceps: An Innovative Technique for Atraumatic Tooth Avulsion” which is also cited on the Wikipedia page dedicated to dental extractions.
For further reading, we recommend the official website extractionwithoutforceps.com, as well as scientific and bibliographic references such as:
- “Lever in tooth extraction. Physical and clinical principles” – Dental Cadmos, Oct 15, 1990;58(15):101–5. PMID: 2279594
- “Forceps in tooth extraction. Method of use and working position” – Dental Cadmos, May 31, 1991;59(9):54–61. PMID: 1864424
To better understand how the EWF technique works, we provide a sequence of images as an example. In the first image, the elevator is inserted beneath a decayed wisdom tooth; extrusion is then performed by repositioning the elevator to manage the progression, and finally the tooth is successfully extracted. All of this takes just a few seconds, with no stress for the patient.
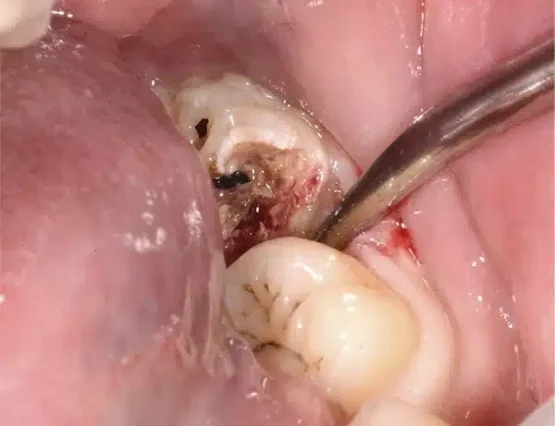
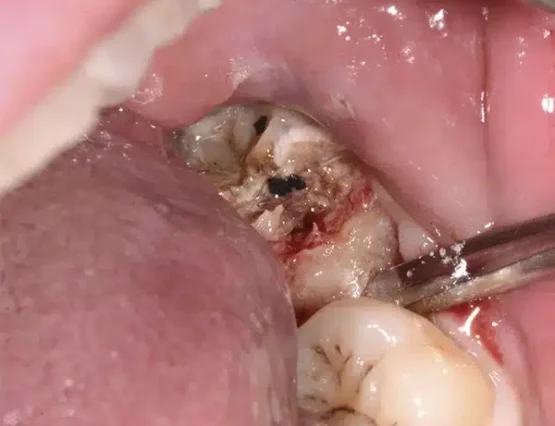
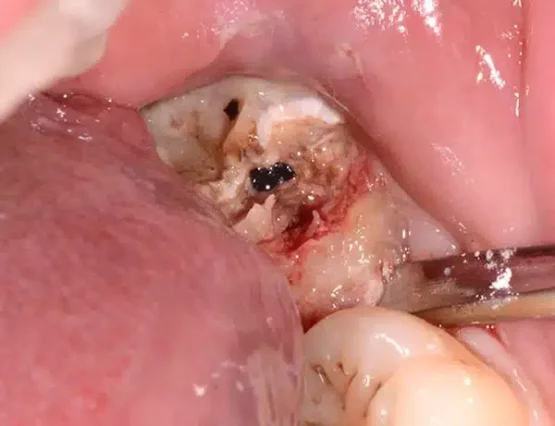
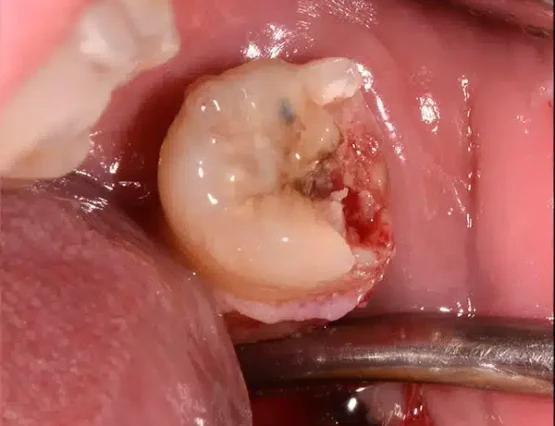
Conscious sedation for extractions
The presence of an anesthesiologist is a valuable asset in our practice. This professional plays a key role in ensuring both patient comfort and safety, as well as supporting the dentist by continuously monitoring vital signs and being ready to intervene in case of emergency.
Sedation involves the administration of sedative medications (either orally or intravenously) to induce a controlled state of relaxation. Depending on the drug used, the method of administration, and the dosage, the depth of sedation can range from mild to moderate (conscious sedation), up to deep sedation or sedation-analgesia. Intravenous conscious sedation in dentistry is the safest and most effective option. Managed by an anesthesiologist, this technique allows the patient to:
- Have little to no memory of the procedure
- Remain awake and cooperative while feeling almost asleep
- Drastically reduce anxiety and emotional tension
- Respond naturally to verbal stimuli
The drugs used in this technique belong to the benzodiazepine family, particularly diazepam (Valium), delorazepam (En), or—very commonly in intravenous use—midazolam, which ensures a rapid onset and optimal recovery.
Conscious sedation equipment
Nitrous oxide (inhalation sedation) has several limitations and provides only mild sedation. It is ineffective for patients with severe dental anxiety, panic attacks, or for long surgical procedures such as implant rehabilitations or wisdom tooth extractions.
Intravenous sedation allows the anesthesiologist to adjust the dosage, achieving even deep sedation when needed. The effectiveness of nitrous oxide depends on the patient breathing consistently through the nose.
If the patient has a cold, breathes through the mouth, cries, or hyperventilates due to fear, the effect of the gas diminishes. Intravenous sedation bypasses this issue, ensuring a stable effect.
Additionally, the nasal mask used for nitrous oxide takes up space on the patient’s face and can interfere with the surgeon’s work.
Finally, in the event of a medical emergency at the chair, an anesthesiologist administering intravenous sedation already has venous access in place, allowing life-saving drugs to be delivered within seconds. With nitrous oxide, this critical access is not available.
Operating microscope
Extracting a wisdom tooth is not just a matter of force, but of extreme precision. The use of an operating microscope during the procedure pushes the boundaries of surgery toward minimally invasive techniques. Why is it essential for third molars? Thanks to high magnification, it is possible to visualize and preserve delicate nerve structures (such as the inferior alveolar nerve) that often run close to the roots.
Better visibility also allows for less bone removal and smaller incisions, preserving healthy tissues. Reduced surgical trauma results in less swelling, less post-operative pain, and a much faster recovery for the patient. The integration of the microscope ensures a level of accuracy that cannot be achieved with the naked eye, making the extraction a truly high-standard surgical procedure.
Sonic surgery for safe extraction of impacted teeth

For complex extractions (impacted teeth or those close to nerves), we use sonic oscillating handpieces. These tips, which move through micro-vibrations (unlike traditional rotating burs), cut bone while preserving nerves and blood vessels. For complex extractions (impacted teeth or those close to nerves), we use sonic oscillating handpieces. These tips, which move through micro-vibrations (unlike traditional rotating burs), cut bone while preserving nerves and blood vessels.By reducing the risk of accidental injury, sonic surgery also allows for micro-regularization of bone walls, stimulating natural bleeding and significantly lowering the incidence of dry socket (alveolar osteitis). Sonic surgery, or piezosurgery, avoids bone trauma by preventing overheating and reducing post-operative swelling. This technique, based on micrometric vibrations, ensures precise cutting, allowing the surgeon to work safely near delicate structures such as the inferior alveolar nerve or the membrane lining the maxillary sinus.
With sonic surgery, the dentist can approach sensitive anatomical structures—like the inferior alveolar nerve—without causing damage. Although it is a much safer technique, no procedure is completely risk-free. For this reason, symptoms must always be carefully monitored, and wisdom tooth removal should be evaluated also in light of potential complications.
Sonic surgery uses a dedicated handpiece with oscillating movements to cut hard tissues (bone and teeth). It selectively acts on mineralized tissues while preserving soft tissues, which remain unharmed even in case of accidental contact. The procedure should always be performed under magnification (such as with a surgical microscope), and nerve and vascular structures must always be carefully avoided, even when using highly safe instruments.
Post-operative protocol
Discomfort and swelling typically last a couple of days, with symptoms gradually improving. The peak usually occurs after 36–48 hours, followed by a steady reduction. It is not normal if pain or swelling increases after 72 hours: this could indicate dry socket due to food accumulation or bone necrosis related to smoking. In these cases, or if fever develops, the dentist should be contacted.
Post-operative management actually begins during the procedure itself. A carefully planned pharmacological protocol may include the use of Soldesam (dexamethasone), injected by the dentist in the surgical area to control edema (swelling) and trismus (difficulty opening the mouth). This injection helps reduce the acute inflammatory response, promoting a more comfortable recovery after wisdom tooth extraction.
Soldesam
Soldesam (dexamethasone sodium phosphate) is a fluorinated corticosteroid commonly used in complex wisdom tooth extractions. The presence of a fluorine atom in its chemical structure makes it more potent than natural corticosteroids such as hydrocortisone, while almost eliminating its ability to retain fluids and salts (mineralocorticoid activity). This allows it to focus primarily on its anti-inflammatory effect. After a complex extraction, injecting Soldesam into the gum tissue around the surgical site helps reduce swelling (edema) thanks to its immediate preventive action. When administered locally, the corticosteroid acts upstream, before inflammation fully develops, effectively blocking the chemical cascade responsible for post-extraction swelling.
Once swelling has already formed, it becomes much harder to reduce and often requires systemic anti-edema medications—which can thus be avoided. Soldesam works by reducing vascular permeability: in simple terms, it “seals” the blood capillaries in the treated area. Normally, after surgical trauma, blood vessels become more permeable, allowing fluids to leak into surrounding tissues and causing swelling. Soldesam prevents this leakage and is applied locally. This targeted injection ensures that a potent dose acts only in the extraction area, avoiding the need for systemic drug administration.
Painkillers and antibiotics may also be prescribed by the dentist to reduce post-operative discomfort and minimize the risk of complications. Recent clinical studies have also introduced biostimulatory protocols to accelerate tissue regeneration and promote faster healing.
L-PRF (Platelet-Rich Fibrin)
After wisdom tooth extraction, it can be beneficial to place membranes obtained from the patient’s own blood (through centrifugation) into the socket. This acts as a natural biological barrier, reducing the risk of infection and accelerating new bone formation.
Laser Photobiomodulation (PBM)
The application of low-level laser light immediately after extraction has shown significant effects in reducing pain and inflammation following wisdom tooth surgery. It also improves local microcirculation and speeds up wound healing.
Practical advice for the patient
The post-operative phase after a surgical procedure such as wisdom tooth extraction is particularly delicate. If sutures are placed, they are usually resorbable and will fall out on their own, or they may be removed at the clinic after about 7–10 days during a follow-up visit. There are several activities to avoid and precautions to follow in order to reduce post-extraction symptoms. Here’s what to do (and what not to do) after a tooth extraction:
Diet after extraction
Whether at breakfast, lunch, or dinner, solid foods—especially hot ones—should be avoided. Soft, cool foods are preferable.
Smoothies, mashed foods, soups, and broths at room temperature are recommended. Very hot foods, exceeding body temperature, can disrupt the blood clot and cause renewed bleeding. Fruit options such as grated apple and mashed banana are also suitable. Alcohol should be avoided.
Protecting the blood clot
During the first 24 hours, avoid vigorous rinsing, do not use straws, and do not suck on the extraction site, as this may dislodge the clot and lead to dry socket.
Chlorhexidine rinses
From the second day, perform gentle rinses with a 0.12% chlorhexidine mouthwash three times a day for one minute, for seven days.
No smoking after extraction
Smoking must be strictly avoided for at least 72 hours, as it significantly delays healing and increases the risk of infection. In particular, tar can adhere to the bone and lead to complications such as dry socket.
Ice after extraction
Ice should be applied in the hours following extraction to reduce swelling, in 15-minute intervals for a few hours.
Alternatives to wisdom tooth extraction
Coronectomy
Patients often consider coronectomy as an alternative to complex wisdom tooth extraction. This surgical procedure involves removing only the crown of the tooth while intentionally leaving the roots inside the alveolar bone. It is performed when radiographic exams (such as Cone Beam CT) show that the roots are very close to the inferior alveolar nerve.
In some cases, removing the entire tooth is not recommended because it may risk damaging the nerve, potentially causing loss of sensation (paresthesia) in the lip or chin. By leaving the roots in place, the infected or problematic crown is removed while minimizing neurological risks. However, if the tooth is no longer vital, the roots cannot be left in the bone, as this could lead to infection.
Orthodontic extraction
In these cases, the tooth is gradually extruded using orthodontic appliances, moving the roots away from the inferior alveolar nerve to allow for a safer and simpler extraction later. For more details, you can refer to our dedicated article on orthodontic-assisted extractions.
Water flosser (oral irrigator)
The water flosser should be directed toward the gum covering the tooth, where a pocket often forms and is difficult to clean during eating and drinking. This can help reduce inflammation and symptoms, allowing the extraction to be postponed. However, the tooth will eventually need to be removed.
Risks and complications of wisdom tooth extraction
The main complication after wisdom tooth extraction is dry socket (alveolar osteitis). This is an inflammation of the bone cavity left after extraction and occurs when the blood clot that forms in the socket is lost.
When the bone is exposed and no longer protected by the clot, it can become contaminated, leading to severe pain, swelling, and bad breath. In the past, even after simple extractions, sutures were often placed. Since the surgical flaps could not be completely closed, the sutures acted as a sort of net to stabilize the clot. However, sutures can actually increase the risk of complications: food can become trapped in the suture mesh during chewing and accumulate in the socket.
Unless a surgical flap has been raised, we now tend to avoid sutures after extraction. To control bleeding, sterile gauze is placed between the teeth to allow a stable clot to form. In my clinical practice, minimizing the use of sutures has reduced the risk of post-extraction bone inflammation by approximately 90% for both upper and lower wisdom teeth.
To prevent complications after wisdom tooth extraction, the procedure should be as atraumatic as possible. The use of elevators instead of forceps reduces the risk of tooth fracture and shortens extraction time. Additionally, the use of vibrating instruments—such as in sonic surgery or piezosurgery—along with sterile saline irrigation, helps reduce the risk of dry socket.
Remove your wisdom teeth quickly and painlessly
Questions and answers about tooth extractions
Extraction and extrusion are not two different procedures for removing wisdom teeth. Extraction is the correct term used to describe the surgical removal of a tooth, while extrusion is an orthodontic term referring to the movement of a tooth outward from the bone..
First of all, because they are difficult to clean properly and to floss. Additionally, chewing mainly involves the second molars, so the natural self-cleaning that normally occurs during chewing does not effectively reach the wisdom teeth. As a result, they are more prone to plaque and tartar buildup, making them more susceptible to decay.
The duration of anesthesia for wisdom tooth extraction is sufficient to cover the entire procedure. It typically lasts between about 1.5 to 3 hours. This allows the gum and the bone around the tooth to remain numb, enabling a pain-free extraction.
This largely depends on the type of extraction and the nature of your job. If your work is physically demanding or involves heavy lifting or exposure to dust/contaminants, it’s best to wait 5 to 7 days. For office-based work, 1 to 2 days are usually sufficient. Always ask your dentist for personalized advice.
We often notice wisdom teeth because they cause pain when they erupt, or when complications arise. Pain may be due to decay reaching the pulp (the nerve) or inflammation of the gum around the tooth. Common symptoms include:
- Swelling
- Gum pain
- Sore throat and white patches
- Ear pain
- Difficulty swallowing
- Difficulty opening the mouth
Problems with wisdom teeth can often spread, causing sore throat, neck pain, earache, and other symptoms. In the presence of necrotic tissue, bad breath may occur due to abscesses or ulcers. For these reasons, extraction of the wisdom tooth may be necessary. Pain involving third molars can be difficult to tolerate, so timely intervention is important to reduce inflammation and address the underlying cause.
Wisdom tooth pain can be related to its development, which usually begins in adolescence, around the age of 17. However, cases requiring extraction due to problems such as decay can occur over a wider age range, typically around 35–40 years, with peaks even at 50 or 60 years. So, wisdom teeth tend to hurt when they are erupting or when they develop decay. At what age should wisdom teeth be removed? It depends on the findings from the patient’s clinical evaluation. Someone who attends regular check-ups every six months can keep the situation under control and decide together with their dentist the best time for extraction.
Advantages of multiple extraction: a single procedure, one recovery period, and often a lower overall cost. Disadvantages: a more demanding recovery and difficulty chewing on both sides. The choice depends on the complexity of the case, the patient’s age, and tolerance. In most cases, no more than two wisdom teeth are removed in a single session; extracting all four at once is generally not recommended due to anesthesia-related limitations.
The gauze placed by the dentist after the extraction is usually kept in place for a few minutes. It depends on the amount of bleeding. With a quick and atraumatic extraction, bleeding is often minimal, so the gauze only needs to be kept in place for a short time.
The cost of wisdom tooth extraction depends on the complexity of the procedure and the initial condition. A simple extraction is less expensive than one involving an impacted upper or lower tooth. At Studio Cozzolino, prices range from approximately €250 to €850 for more complex cases. Costs vary because wisdom teeth are generally more difficult to remove. Lower wisdom teeth are typically more complex than upper ones, as the upper jaw bone is softer, allowing for easier extraction. If conscious sedation is required, an additional cost of €700 is applied.
In the first and third trimesters, extraction is usually postponed. In the first trimester, because it is the most delicate phase of fetal development; in the third, because the patient’s position and the stress of the procedure may cause unnecessary discomfort. If the procedure is necessary, the safest time is the second trimester. During this period, the safety margin is higher, and standard local anesthetics are commonly used without issues in everyday clinical practice.
Wisdom tooth extraction is carefully planned using radiographic imaging before the procedure. This allows the clinician to define the appropriate technique and anesthesia in order to minimize discomfort for the patient. However, unexpected factors can always occur, potentially prolonging the procedure and making it more complex, which may result in increased discomfort.
Post-operative pain after wisdom tooth extraction usually appears once the anesthesia wears off and is managed with painkillers prescribed by the dentist, helping control discomfort during the day and at night. Typically, it resolves within a few days. If pain reappears or persists after a month, it is advisable to contact your dentist for a check-up.
No, removing wisdom teeth does not change the shape of your face. Any temporary change in appearance is usually due to swelling, which resolves within a few days.
As mentioned, wisdom tooth extraction itself does not affect pain perception, since local anesthesia eliminates pain during the procedure. However, lower wisdom teeth extractions can be more complex due to their position and the denser bone. They are also more often impacted and may be close to the inferior alveolar nerve, which can make the procedure more technically demanding.
Do you want to extracted without pain? Contact us today.
Our team is available to assist international patients, provide clear information, and support you before and during your visit to Naples.
- Phone: +39 081 245 1805
- Email: info@studiodentisticocozzolino.it
- Address: Via Raffaele De Cesare 31, 80132 – Naples, Italy
We recommend contacting us in advance to better organize your visit and ensure the best possible care. Ask for info or schedule a visit.